Cancer and Cannabis: Palliative and Antitumor Effects
By Diana Hahn and Stacey Marie Kerr, MD
sorting through headlines
Considering the media buzz around cannabis and cancer, we strongly urge patients and their doctors to base treatment choices on evidence-based science rather than personal opinions, headlines, or hearsay.
There is clear evidence that cannabinoids can be an effective palliative care option for cancer patients, however whether "cannabis cures cancer" is a complex topic with lots of promise, many unknown variables, and as yet, little conclusive evidence.
For example, a recent study has shown that cancer patients who use cannabis have a significantly lower in-hospital mortality rate with decreased incidence of heart failure or cardiac disease. the same study reported, however, that cannabis users had a slightly increased incidence of strokes while in hospital. [1] Studies like this one highlight the need for further research so we may understand the science behind the statistics.
Palliative Care
For many cancer patients, the side effects of treatment (e.g. chemotherapy and radiotherapy) may feel as debilitating as the disease itself. Palliative care affords people comfort, higher quality of life, and may even support healing by improving sleep and attitude as well as allowing patients to continue treatment programs that might otherwise be intolerable. Cannabinoids have been shown to help with several common adverse symptoms of cancer and cancer treatments.
| Side Effect/Symptom | % of Patients with cancer who experience symptoms |
|---|---|
| Weight Loss | >50% |
| Wasting Syndrome (Cachexia) | ~50% |
| Early Satiety/Decreased Appetite | ~50% |
| Moderate to Severe Pain | 33% |
| Anxiety or Depression Requiring Treatment | 33% |
| Acute Nausea and/or Vomiting | 30% |
Weight Loss and Wasting Syndrome (Cachexia)
Appropriate varieties of cannabis help with weight loss and wasting syndrome by increasing appetite. There are many anecdotal stories about cannabis making food taste better, with clinical evidence supporting patients’ experiences. CB1 receptors are involved in the motivational and reward aspects of eating, and anandamide binding to these receptors has been shown to increase appetite. Cannabis literally makes food taste better, incentivizing people to eat more. [2] One study showed that cannabis increased appetite by 49%, but also showed that Megestrol (a progesterone pharmaceutical drug) increased appetite even more. [3] One possible benefit of cannabis that this study did not take into account, however, is that that cannabis may provide therapeutic effects for multiple symptoms, allowing a patient to take one drug instead of several.
Nausea and Vomiting
Cannabinoids appear to consistently outperform placebo as well as pharmaceutical anti-nausea drugs in treating chemotherapy-related nausea and vomiting. In one study, oral THC was shown to be more effective than placebo or prochlorperazine (Compazine). In another study, THC was shown to be more effective than phenothiazines (Compazine falls into this category of drugs) and metoclopramide (Reglan). [2]
For most patients, 10-40 mg of THC/day controls nausea and vomiting. [4] Although THC seems to be the cannabinoid that effectively treats nausea, patients may choose to take CBD with THC to lessen the side effects of pure THC (mainly increased psychoactivity).
It is important to note that the delivery method may make a difference in efficacy for some patients, especially since nausea and vomiting may make oral consumption of medicine difficult. While the Department of Health does not condone smoking, smoking or vaporizing cannabis provides fast relief and was actually found to be more effective than oral THC in the first study mentioned. Aside from inhalation, suppositories may be an effective delivery method for patients with nausea. Suppositories may also have the added benefit of reducing the psychoactivity of THC.
Pain
Treating pain with cannabinoids is a fairly well documented topic. Specifically regarding cancer pain, studies have shown that a 1:1 THC to CBD ratio was effective in treating neuropathic pain related to chemotherapy in 1 out of 5 patients. [2] This response was enough to consider cannabinoids an effective treatment option for cancer pain, especially in light of the efficacy rate and side effects of other pain treatment options. Animal studies have also shown that CBD pre-treatment can actually prevent chemotherapy induced neuropathic pain. [2]
Cannabis may also be combined with opioids to treat pain, and has been proven to be safe when taken in combination with oral sustained release opioids (i.e. oxycodone and morphine). [2] In general, cannabinoids enhance the analgesic (pain killing) effects of opioids, and many patients find they can lower their opioid doses when concurrently using cannabis medicines.
Anxiety and Depression
Euphoria is often considered a side effect of cannabis, however in people who are dealing with anxiety and/or depression, euphoria can be a desired therapeutic effect of cannabis treatment. Aside from euphoria, cannabis also helps patients sleep better, which may result in a better mental state with less anxiety and depression.
Antitumor Activities
In preclinical studies, cannabinoids have exhibited antitumor activity. It is important to note that cannabinoids have also exhibited pro-tumor activity in certain situations. [6] Currently cannabis is generally considered a safe treatment for cancer patients, with the potential pro-tumor qualities of cannabinoids not outweighing the benefit of using cannabis as a palliative treatment for cancer. This is especially true if other drugs do not work adequately or are intolerable.
The outlook for endocannabinoid system-based antitumor treatments is promising, however there are still many unknowns and paradoxes for us to understand. There are three primary mechanisms we know of that cannabinoids and the endocannabinoid system are involved in tumor suppression (or growth): apoptosis, angiogenesis, and metastasis. All the information presented here comes from work done in labs (not with human patients), is for informational purposes only, and does not represent a professional medical opinion.
Apoptosis
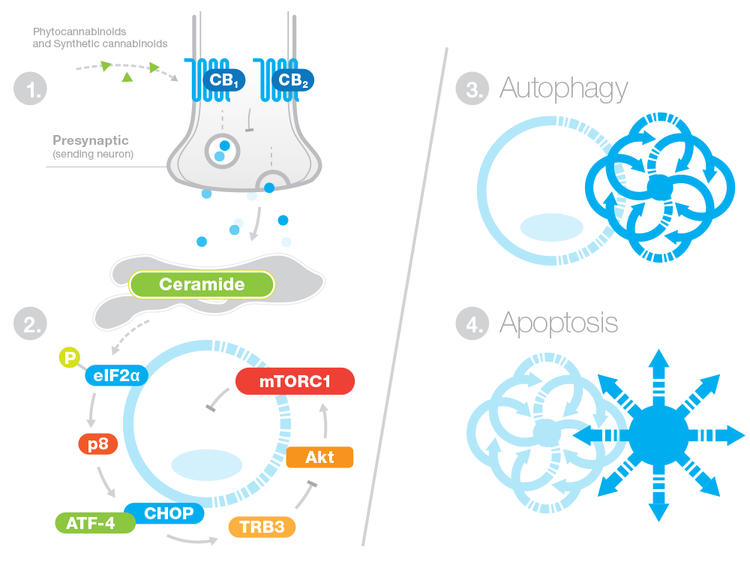
Apoptosis is a process of programmed cell death. Cannabinoids encourage apoptosis in cancer cells through a process called autophagy. In other words, when cannabinoids bind to cannabinoid receptors as agonists, they set off a chain reaction, or mechanism, that leads to cell death (see image below). [4] Some cannabinoid receptor agonists are more effective than others in inducing cancer cell apoptosis. For example, THC has been shown to be more effective than synthetic cannabinoids, even if it has a lower binding affinity for CB1 and CB2. [5]
Scientists are still studying to discover which cannabinoid receptor—CB1, CB2, or both—is involved in leading to apoptosis. CB1 and CB2 receptors are present in many types of cancer cells, even if they are not present in the healthy tissue from which the cancer originated. So far, lab tests have shown that blocking CB2 receptors in pancreatic, breast, and hepatic cancer cells inhibits cannabinoid-induced apoptosis, implicating CB2 as the active receptor in apoptosis. Blocking both CB1 and CB2 receptors in gliomas inhibits cannabinoid-induced apoptosis, suggesting that both or either is involved. [5] So while we know that different receptors are involved in different cancers, this information simply increases the need for more research.
CBD and other cannabinoids also appear to support apoptosis independent of CB1 and CB2 receptors. Scientists have proposed that CBD increases the production of reactive oxygen species in breast cancer cells, causing damage that leads to their destruction. [5] CBD has also been observed activating receptors known as “TRPV2” in aggressive glioma cells (brain cancer), and when these are activated, the glioma cells are significantly more vulnerable to chemotherapeutic agents.
Interestingly, cannabinoids behave differently in healthy cells, where they may actually extend the life of a cell rather than cut it short. [5] Cannabinoid anti-inflammatory and antioxidant activity in healthy cells may also support limiting the growth and spread of tumors. [2] In preclinical studies, cannabinoids have been shown to kill the following types of tumors:
Lung, breast, colorectal, pancreatic
Hepatocellular (liver)
Skin carcinoma and melanoma
Thyroid epithelioma
Lymphoma
Glioma
Cannabinoids bind to CB1 and CB2 receptors. This binding activates a series of reactions that induce autophagy of the cancer cell. Autophagy is the protective process our body uses on all damaged cells, degrading old cellular components, and then recycling them to form useful nutrients and energy. In the case of cancer and cannabinoids, the cannabinoids trigger first, autophagy of tumor cells, which then leads to apoptosis (programmed total cell-death) of the cancer cell.
Angiogenesis
Angiogenesis refers to the growth and development of blood vessels. In cancers, angiogenesis is the growth of blood vessel networks that feed tumors, allowing them to use nutrients from the body to grow. Cannabinoids inhibit tumor angiogenesis by blocking the activation of vascular endothelial growth factor (VEGF). This anti-angiogenesis activity has so far been shown in relation to gliomas and thyroid carcinomas.
Metastasis
Metastasis refers to the migration and proliferation of cancer cells in a part of the body separate from the original tumor. THC reduces the formation of new tumors in animal models by activating CB1 and/or CB2 receptors. More specifically, cannabinoid receptor agonists have been shown to inhibit adhesion, migration, and invasiveness of glioma, breast, lung, and cervical cancer cells in culture. [5]
CBD has also been shown to reduce the invasiveness and metastasis of tumors independent of CB1 and CB2 receptors. CBD is known to inhibit a cancer gene and protein Id-1 which is a key regulator of the metastatic potential of cancers, expressed in some hormone-independent breast cancer cells. By inhibiting Id-1, CBD inhibits the metastasis of aggressive breast cancers; researchers expect to find CBD doing the same in ovarian carcinomas, melanomas, and several other malignancies where Id-1 is found. [5]
Cancer Types and Endocannabinoid System Effects
| Tumor Type | CB Receptors or ECB degrading enzymes | References |
|---|---|---|
| Hodgkin lymphoma | CB1 levels increased | (Benz et al., 2013) |
| Non-Hodgkin lymphoma | CB1 levels increased | (Gustafsson et al., 2008) |
| Chemically-induced cellular hepatocarcinoma | CB1 levels increased | (Mukhopadhyay et al., 2015) |
| Hepatocellular carcinoma | CB1 and CB2 expression correlates with improved prognosis of patients with hepatocellular carcinoma | {Xu, 2006 #378} |
| Human epithelial ovarian tumors | CB1 levels increased. Correlation with disease severity | (Messalli et al., 2014) |
| Stage IV colorectal cancer | CB1 levels are a factor of bad prognosis following surgery | (Jung et al., 2013) |
| Colon cancer | CB1 levels decreased, CB1 genetic ablation increased the growth of colon carcinomas | (Wang et al., 2008) |
| Pancreatic cancer | CB1 and CB2 levels increased and MAGL and FAAH levels decreased | (Michalski et al., 2008) |
| Prostate cancer | CB1 levels increased associated with severity of disease and poor prognosis | (Chung et al., 2009) |
| Prostate cancer | FAAH tumor levels (but not CB1) directly correlate with severity of the disease | (Thors et al., 2010) |
| Breast cancer | CB2 levels increased. Correlation with disease severity | {Caffarel, 2010 #15; Caffarel, 2006 #16; Perez-Gomez et al., 2015 #349} |
| Glioma | CB2 levels increased with degree in gliomas | (Sanchez et al., 2001) |
| Mantle cell lymphoma | CB1 and CB2 levels increased and FAAH levels decreased | (Ek et al., 2002; Islam et al., 2003; Wasik et al., 2011) |
| UV light induced skin carcinogenesis | CB1 and CB2 genetic ablation decrease UV light induced skin carcinogensis | (Zheng et al., 2008) |
| Leukemia | CB2 overexpression enhances the predisposition to leukemia after leukemia virus infection. | (Joosten et al., 2002) |
| Glioma, breast cancer, skin cancer | GPR55 increased levels associated with higher histological tumor grade | (Andradas et al., 2011; Perez-Gomez et al., 2013) |
Complimentary vs. Alternative Treatment
Many patients have found cannabis to be an effective complimentary medicine in treating cancer, meaning that they continue their other treatments while also using cannabis. While some patients use cannabis strictly for palliative care, others choose to take higher doses of cannabinoids as an adjuvant therapy on top of conventional treatment options.
Cannabinoids are generally considered safe to take in combination with conventional antitumor drugs as well as opioids, although dosages of opioids may need to be decreased when used in combination with cannabis. Cannabinoids target different receptors than conventional chemotherapy drugs and have low toxicity effects when used with these agents. [4] Opioids in combination with cannabis have also proven to be safe, with cannabis potentially increasing the efficacy of opioids. [2]
It is important to note that malignant tumors are unique, with tumors expressed differently in different parts of the body, as well as from person to person, even if comparing the same kind of cancer across individual patients. Much of cancer research has focused on identifying specific markers, and targeting precise mechanisms and biological pathways. This type of specialization requires a high level of understanding and an ability to match a patient’s markers with the correct treatment. Currently we do not yet know what the particular markers are that would make patients good candidates for cannabinoid-based antitumor treatment.
Using cannabis as an alternative therapy while forgoing conventional therapies is a high-risk choice. Although there is preclinical evidence that cannabinoids kill cancer, there is no proven clinical evidence that cannabinoids alone are effective enough to bring a patient to remission. It is important for patients to keep in mind that for all the anecdotal success stories of using cannabis as an alternative therapy for cancer, there are also stories from patients with treatable cancers who have refused conventional treatment, had tumors progress while using cannabis, and have found themselves in a much worse situation than when they were diagnosed. The latter type of story is far less glamorous or inspirational, but it is important for patients to be realistic and weigh the risks and benefits of all treatment options.
Sources:
Vin-Raviv N, et al. Marijuana use and inpatient outcomes among hospitalized patients: analysis of the nationwide inpatient sample database. Cancer Medicine. 21 October 2016. doi: 10.1002/cam4.968
Abrams DI and Guzman M. Cannabis in Cancer Care. Clinical Pharmacology & Therapeutics, Volume 97 Number 6, June 2015, doi:10.1002/cpt.108
Ben Amar. Cannabinoids in medicine: A review of their therapeutic potential, J Ethnopharmacology Volume 105, 21 April 2006
Hospodor AD. Cannabinoids as an adjuvant therapy for pancreatic cancer. [abstract]. In: Proceedings of the AACR Special Conference on Pancreatic Cancer: Innovations in Research and Treatment; May 18-21, 2014; New Orleans, LA. Philadelphia (PA): AACR; Cancer Res 2015;75(13 Suppl):Abstract nr B83.
Velasco G, Sanchez C, and Guzman M. Anticancer Mechanisms of Cannabinoids. Current Oncology. Mar; 23(S2): S23-S32 (2016).
Velasco, G., et al. The use of cannabinoids as anticancer agents. Prog Neuro-Psychopharmacol Biol Psychiatry (2015)
Arney, K. Cannabis, Cannabinoids, and Cancer—The Evidence So Far. http://scienceblog.cancerresearchuk.org/2012/07/25/cannabis-cannabinoids-and-cancer-the-evidence-so-far/
Hospodor A. Cannabis Dosages for Cancer Presentation.