Does Cannabis Help with Glaucoma?
By Diana Hahn and Stacey Marie Kerr MD
Glaucoma and the roots of MMJ
There have been many new developments and discoveries regarding cannabis as medicine in the last decade, but the vast majority of this progress has been outside our understanding of cannabis in relation to glaucoma.
Cannabis as a treatment for glaucoma became known in the 1970s due to a few highly publicized case studies like that of Robert Randall, who was the first federally recognized medical marijuana patient with glaucoma in the United States post cannabis prohibition. Today, glaucoma frequently appears on lists of qualifying conditions for state medical cannabis laws, but how effective is cannabis based on the current evidence?
Glaucoma 101
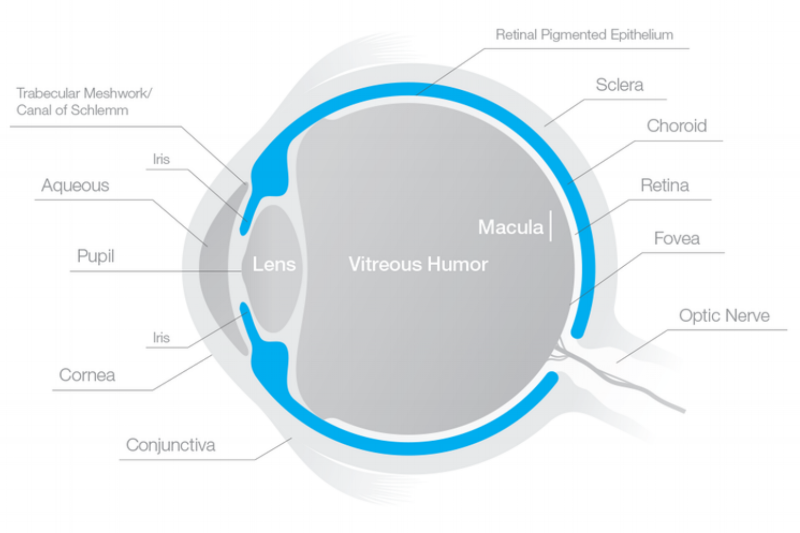
Glaucoma is a group of diseases that damage the eye’s optic nerve, and can sometimes result in loss of vision or blindness. The most common cause of nerve damage is high intra-ocular pressure (IOP), caused by blockages in the flow-path of aqueous humor (fluid) in the eye. The blockage causes a buildup of aqueous humor, creating pressure that damages the vulnerable optic nerve. Many current treatments for glaucoma involve improving the appropriate flow of fluid within the eye and/or lowering IOP.
Circulation of fluid in a normal eye. The aqueous humor is secreted by the ciliary body, then it passes through the pupil into the anterior chamber, finally draining through the trabecular meshwork located in the angle between the cornea and the iris. CB1 receptors are present in several areas of the eye, including the ciliary body and the trabecular meshwork.
cannabinoids as a treatment
Although there is accepted documentation that cannabinoids do lower the pressure inside the eye and may have neuroprotective effects, challenges with delivery methods and side effects have prohibited cannabis from being a first-line treatment for glaucoma. Still, there are patients for whom conventional treatment is intolerable or ineffective. For these patients, cannabis may be appropriate.
Lowering IOP
A study in 1971 showed that smoking cannabis lowers IOP by 25-30% with effects lasting for 3 to 4 hours. More recent studies have shown that THC, CBD, and CBG in particular lower IOP through a local mechanism in the eye rather than through the central nervous system. [1]
CB1 receptors have been found in many parts of the eye including the ciliary epithelium, the trabecular meshwork, Schlemm’s canal, ciliary muscle, ciliary body vessels, and retina. [1] Although we do not have definitive evidence of how the endocannabinoid system modulates IOP, some proposed theories based on cannabinoid receptor distribution include:
Affects the production of aqueous humor
Inhibits aqueous humor build up via calcium influx inhibition
Affects aqueous humor outflow
Vasodilates blood vessels, improving aqueous humor drainage
Exerts influence through a prostaglandin mediated mechanism. [1]
Neuroprotection
Vision loss is caused by apoptosis, or cell death, of optic nerve cells. In glaucoma, apoptosis is caused by compression due to high IOP and/or ischemia due to lack of blood flow. [1] In ischemia, lack of blood flow triggers the release of the neurotransmitter glutamate, which causes a chain reaction ending in apoptosis (cell death). THC has been shown to block the release of glutamate by activating CB1 receptors. [1] In addition, both CBD and THC have been shown to have antioxidant properties, which may further protect against nerve cell death.
how to's: delivery method, dose, and side effects
Delivery Method: Although smoking and oral delivery have shown to be effective, topical application would be ideal for glaucoma in order to concentrate the desired effects in the eye and limit systemic effects (see Side Effects). Creating a topical application has proven to be difficult, because cannabinoids are lipophilic (fat soluble) and do not dissolve well in water-based solutions. Mineral oil-based solutions have been tried, but they proved to be eye irritants. Work continues in cannabinoid science and technology that may allow for a cannabinoid topical eye solution in the future. [1]
Dosing: Treating glaucoma largely depends on keeping IOP at an acceptable level at all times. Based on the research that has been done, cannabinoids would need to be administered every 3 to 4 hours throughout the day and night. While some patients may choose to smoke during the day, it is highly undesirable to wake up every few hours throughout the night to medicate. Currently, other medications can be taken with less frequency with the same efficacy.
Side Effects: Aside from reducing IOP, cannabis may also cause redness, reduced tear production, and change in pupil size in the eye. Common side effects of cannabis include sleepiness, euphoria/dysphoria, reduced coordination, warped sense of time, and memory and cognition impairments. Acute side effects of cannabis observed in glaucoma patients include increased heart rate and lowered blood pressure. [2] It is important to note that lowered blood pressure has been identified as a risk factor for glaucoma as it may compromise blood flow to the optic nerve. [3] Patients using cannabis to treat glaucoma should be aware of this and monitor their blood pressure to see if they regularly experience this side effect.
Sources:
Tomida I, et al. Cannabinoids and Glaucoma. Br J Ophthalmol 2004; 88:708-713 doi:10.1136/bjo.2003.032250
Merritt J, et al. Effect of Marihuana on Intraocular and Blood Pressure in Glaucoma. Opthamology. Volume 87, Number 3. March 1980.
Complimentary Therapy Assessment Marijuana in the Treatment of Glaucoma. American Academy of Opthamology. May 2003